NHS hospitals and GP practices are failing to carry out routine HIV testing
By Will Stroude
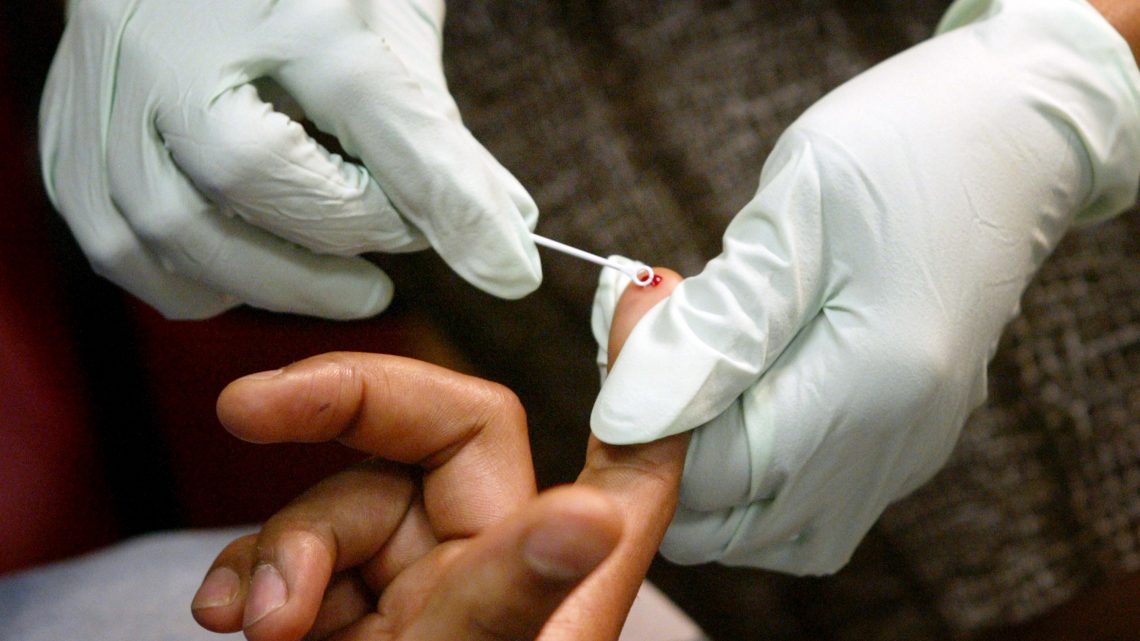
Hospitals and GP practices are reportedly failing to carry out routine HIV testing on new patients and those admitted to hospital.
In 2013, experts recommended that in areas where more than two in 1,000 people live with HIV everyone who registers with a GP in the area or is admitted to a local hospital is given a HIV test.
However, many NHS providers aren’t doing so, the BBC reports.
A BBC investigation discovered that 82% of hospitals in high-prevelance areas across england were not offering these routine tests in accordance with the 2013 guidelines, while 70% of local authorities in high-prevalence areas were not funding all GP surgeries to test new patients.
Responding to the findings, Dr Chloe Orkin, of the British HIV Association, said: “Testing for HIV is very cost-effective. Deaths due to late diagnosis are completely preventable through excellent treatments.”
With around 17% of people who are living with HIV not aware of their status and not on medication, a lack of routine testing may be aiding the spread of the virus.
Kat Smithson, Policy and Campaigns Manager at NAT (National AIDS Trust), described the findings as “a great shame.” In a statement, she wrote: “Back in 2014/15 NAT found that only a quarter of local authorities with a high prevalence of HIV were commissioning HIV testing in GP surgeries and even fewer in hospital settings.
“This data shows only a slight increase in commissioning of these testing services in the past year. It’s a great shame that people still cannot access testing as standard in these settings.
“Testing for HIV in GP surgeries and on admission to hospital has enormous potential to reach people who wouldn’t otherwise test, and to diagnose people earlier. All too often when people are diagnosed with HIV it turns out we’ve missed these vital opportunities somewhere along the way.”
“One thing commissioners of testing told us back in 2015 is that making the funding available for testing doesn’t translate to it being used. There still seem to be significant barriers to normalising testing for HIV in medical settings outside the GUM clinic.
“Sometimes medical staff don’t feel confident offering the test or don’t see it as relevant. We need to identify these barriers and deal with them to normalise testing. HIV testing is not expensive, but it can have a significant impact if more people are diagnosed on time and are on treatment.”
A Department of Health representative for England said: “Over the next five years, we will invest more than £16bn in local government public health services.
“While councils have had to make savings, they have also shown that good results can be achieved at the same time, and are best placed to understand where money is best spent”.
More stories:
More straight guys are watching gay porn than you might think
Gus Kenworthy celebrates National Coming Out Day with a kiss – and an important message
